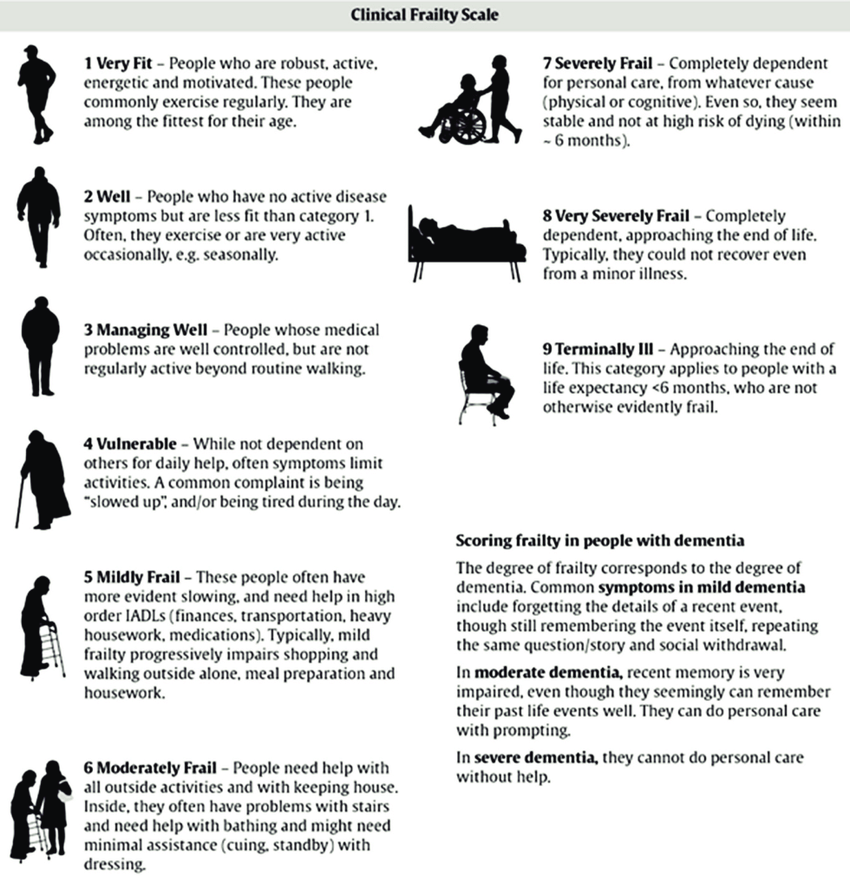
The Clinical Frailty Scale (CFS), developed by Dr. Kenneth Rockwood, is a 9-point clinical tool used to assess how fit or frail an older adult is — based on their functional independence, not their age. In Singapore, where one in four residents will be aged 65 and above by 2030, the CFS is used by geriatricians, physiotherapists, and occupational therapists to guide treatment decisions, set rehabilitation goals, and identify when community-based support is needed. A score of 1 to 3 indicates fitness; 4 to 6 indicates increasing vulnerability; 7 to 9 indicates severe or end-stage frailty.
Why Age Alone Is Not a Good Measure of Health
Two people aged 80 can present completely different clinical pictures. One may still be hiking on weekends. The other may need assistance getting out of a chair. Chronological age tells you very little about either of them.
This was the insight that drove Dr. Kenneth Rockwood, a geriatrician and professor at Dalhousie University, to develop the Clinical Frailty Scale in the early 2000s. Rather than treating age as a proxy for health, the CFS assesses a person’s actual functional reserve — their physical capacity, activity level, and independence in daily life.
The result is a 9-point scale, from “Very Fit” (1) to “Terminally Ill” (9), that gives clinicians and families a shared language for something previously difficult to quantify: the difference between ageing well and becoming frail.
What the Clinical Frailty Scale Scores Mean
Each score on the CFS corresponds to a description of function and independence:
- Score 1 — Very Fit: Robust, active, motivated. Exercises regularly.
- Score 2 — Well: No active disease symptoms, but less fit than score 1.
- Score 3 — Managing Well: Medical conditions are controlled. Activity is limited to walking.
- Score 4 — Vulnerable: Not dependent on help yet, but symptoms limit activity. Tires easily.
- Score 5 — Mildly Frail: Slowed. Needs help with higher-level functions (finances, transportation, heavy housework).
- Score 6 — Moderately Frail: Needs help with outside activities and some household tasks.
- Score 7 — Severely Frail: Fully dependent on others for personal care. Stable, not at high risk of dying.
- Score 8 — Very Severely Frail: Completely dependent and approaching end of life.
- Score 9 — Terminally Ill: Life expectancy under 6 months, regardless of frailty.
The clinical significance of each score is not just descriptive — it determines what kind of intervention is appropriate, and how aggressively a team should pursue recovery versus quality of life.
How the Clinical Frailty Scale Is Used in Clinical Practice
Doctors and Specialists
Physicians use the CFS to guide high-stakes decisions around surgery, medication tolerance, and intensity of treatment. A patient scoring 1 or 2 may be a strong candidate for an elective procedure. A patient scoring 6 or 7 may need a more conservative approach, with goals shifting toward comfort and quality of life rather than aggressive intervention.
In Singapore’s restructured hospitals and specialist clinics, the CFS is increasingly used as a standard intake assessment for older patients — particularly in emergency, surgical, and oncology contexts.
Physiotherapists
For physiotherapists, the CFS score shapes the entire rehabilitation programme. A patient assessed as mildly frail (score 5) still has meaningful potential to regain strength and balance. The physiotherapist designs a targeted exercise plan — often incorporating progressive resistance training, balance work, and functional mobility — aimed at preventing progression to a higher frailty score.
At scores 6 and above, the physiotherapy focus shifts toward safe mobility, fall prevention, and maintaining whatever function remains. Our clinicians at Lifeweavers have managed these cases in acute hospital settings and have built years of experience practicing in the community — which means we understand the full trajectory, not just the snapshot.
Occupational Therapists
OTs approach the CFS through the lens of Activities of Daily Living (ADLs). A score of 6 — moderately frail — means the person needs help with housework and outside activities but can still manage personal care. The OT’s intervention at this level focuses on home modifications, adaptive equipment prescription, energy conservation strategies, and caregiver training to extend independent function for as long as possible.
A higher score may indicate the need for more intensive home support, equipment such as hospital beds or ceiling hoists, or a structured home-based rehabilitation programme.
The Clinical Frailty Scale and Frailty Prevention in Singapore
Singapore’s ageing trajectory makes frailty prevention a national priority. The Agency for Integrated Care (AIC) and the Ministry of Health have both emphasised active ageing and early intervention as cornerstones of the national strategy for eldercare.
What the CFS adds to this picture is precision. Rather than waiting for a fall, a hospitalisation, or a crisis to prompt intervention, the scale allows families and clinicians to identify the early warning signs of functional decline — often years before a person becomes fully dependent.
A parent who shifts from score 3 to score 4 between annual reviews has not simply “got a year older.” They have crossed a threshold from managing well to becoming vulnerable. That is the moment to act: to assess, to intervene, and to build the support systems that slow the slide.
This is exactly why frailty assessment connects directly to programmes like falls prevention, Parkinson’s disease management, stroke recovery, and dementia maintenance — all of which address conditions that both cause and accelerate frailty.
Can Families Use the Clinical Frailty Scale at Home?
The CFS is widely reproduced online — including the NHS Specialised Clinical Frailty Network version — because its visual format makes it accessible to non-clinicians. Families can use the descriptions as a rough reference point.
If you notice that a parent who was “managing well” last year now tires after short walks, avoids social outings, or is struggling with tasks they previously handled independently, the CFS offers a structured way to frame what you are observing. It gives you language to bring to a doctor or therapist appointment.
However, self-assessment has real limitations:
Nuance and baseline accuracy. A registered therapist distinguishes between someone’s usual baseline and a temporary dip due to illness or pain. Getting the score wrong in either direction leads to under- or over-treatment.
Hidden contributors. Clinicians assess factors that are not visible in a brief observation: sarcopenia (muscle loss), cognitive changes, nutritional status, polypharmacy risks. These all influence frailty and must be assessed properly.
What to do with the score. Knowing a number is only useful if it leads to action. A therapist builds the intervention plan — the targeted exercises, home adaptations, caregiver supports, and monitoring schedule — that turns the score into a roadmap.
Use the CFS as a prompt, not a verdict. If something has changed, that is your signal to seek a professional assessment.
How Lifeweavers Assesses and Responds to Frailty
At Lifeweavers, frailty assessment is embedded into how our multidisciplinary team approaches older adult rehabilitation. Whether a client comes to us following a hospitalisation, a fall, a new diagnosis, or simply because a family member has noticed a decline, we build our programme around where that person actually is — functionally, cognitively, and socially.
Our physiotherapists, occupational therapists, and care coordinators work together from the initial assessment, using tools like the CFS alongside other clinical measures to build a programme that is realistic, progressive, and genuinely person-centred.
If you are concerned about a loved one’s frailty level, or want to understand what rehabilitation options are available, speak to our team via WhatsApp Live Chat.
References

