Insurance & Rehab Therapy: Navigating Coverage in Singapore’s "New Normal" in 2026
Singapore’s healthcare landscape has shifted from “Lifespan” (living longer) to “Healthspan” (living well). While our medical system is world-class, many Singaporeans are surprised to find a “rehab gap” when they leave the hospital. This guide clarifies exactly what your insurance covers when you transition from a hospital bed to home-based or clinic-based recovery.
Quick Takeaways:
The Baseline: MediShield Life covers acute hospital stays but offers minimal support for private outpatient or home-based rehab.
The Key: Integrated Shield Plans (ISP) are the primary path to private, holistic rehab (Physiotherapy, Occupational, Speech Therapy).
The 5% Rule: New 2026 regulations require a 5% co-payment, usually capped at $3,000/year if using panel providers and pre-authorisation.
The Cost of Waiting: Uninsured comprehensive rehab can cost $3,000 to $10,000+ per month. Early intervention prevents long-term disability and higher future costs.
- Eligibility: Only for Singaporeans and PRs (Expats can buy private-only plans, but “Integrated” Shield Plans are specifically for those with MediShield Life).
- Pro-Tip: Don’t Wait for a Referral: Many private specialists focus on the surgery or the acute “fix” and may not realize the intensity of rehab required for a full recovery. You are entitled to request a specific referral. If you want a multidisciplinary program (Physio, OT, Speech), ask your specialist for a “Comprehensive Post-Hospitalisation Rehabilitative Therapy” referral. This ensures your Integrated Shield Plan covers the full scope of your recovery, not just a few generic sessions.
Table of Contents
Navigating the 2026 Insurance Landscape
The rules for private health insurance in Singapore underwent a significant shift on April 1, 2026. If you are planning for rehabilitation – whether for a stroke, major surgery, or a chronic condition – understanding these updates is the difference between a fully funded recovery and unexpected financial stress.
At Lifeweavers, we advocate for “Healthspan” (living well) rather than just lifespan. To achieve this, you must know how to leverage your insurance “toolbox” to cover the gap between hospital discharge and a full return to independence.
The 3 Tiers of Rehab Coverage in Singapore
To plan your recovery effectively, you must understand the three layers of the Singapore healthcare safety net.
1. MediShield Life (The Baseline)
MediShield Life is the mandatory national plan. While it covers inpatient hospital stays, its outpatient rehab support is limited. In 2026, it covers Community Hospital rehabilitative stays at a rate of approximately $370 per day. However, it offers zero coverage for private outpatient clinics or home-based therapy sessions.
2. Integrated Shield Plans (IPs) & Riders (The Gold Standard)
This is the primary path to private, high-quality rehab. Most IPs cover post-hospitalisation treatment for a period of 90 to 365 days after discharge. This allows you to access specialised services like those at Lifeweavers, provided they are related to your hospital stay.
3. CareShield Life (The Long-Term Payout)
For those facing long-term disability (unable to perform 3 out of 6 Activities of Daily Living), CareShield Life provides a monthly cash payout – starting at $689/month in 2026. Because this is a cash payout, it can be used to fund long-term “maintenance” therapy that standard hospital insurance typically stops covering.
Why an Integrated Shield Plan is a “Cashless” Necessity in 2026
For most Singaporeans, the biggest fear of private rehab is the “cash drain.” However, the Integrated Shield Plan (ISP) remains the most cost-effective tool because of its unique relationship with MediSave.
While all Singapore Citizens and Permanent Residents (PRs) are eligible for an IP, the strategic advantage lies in the Additional Withdrawal Limits (AWLs). In 2026, you can use your MediSave to pay for your IP premiums up to a cap (e.g., $600/year for those aged 41-70), meaning the “private” upgrade often requires zero to minimal cash top-up for many age groups.
More importantly, under the new 2026 rules, while you must now bear the 5% co-payment and the deductible, both can be fully paid using MediSave (subject to MOH withdrawal limits). At Lifeweavers, we find that clients with a proper ISP and Rider are able to fund the most crucial part of their rehab journey – immediately after discharge for up to one year – without ever touching their bank savings, effectively “rivalling” expensive international plans that require high cash premiums.
The 2026 Reform: The 5% Co-payment & $6,000 Cap
As of April 2026, the Ministry of Health (MOH) has updated the framework for Integrated Shield Plan riders to encourage sustainable healthcare spending.
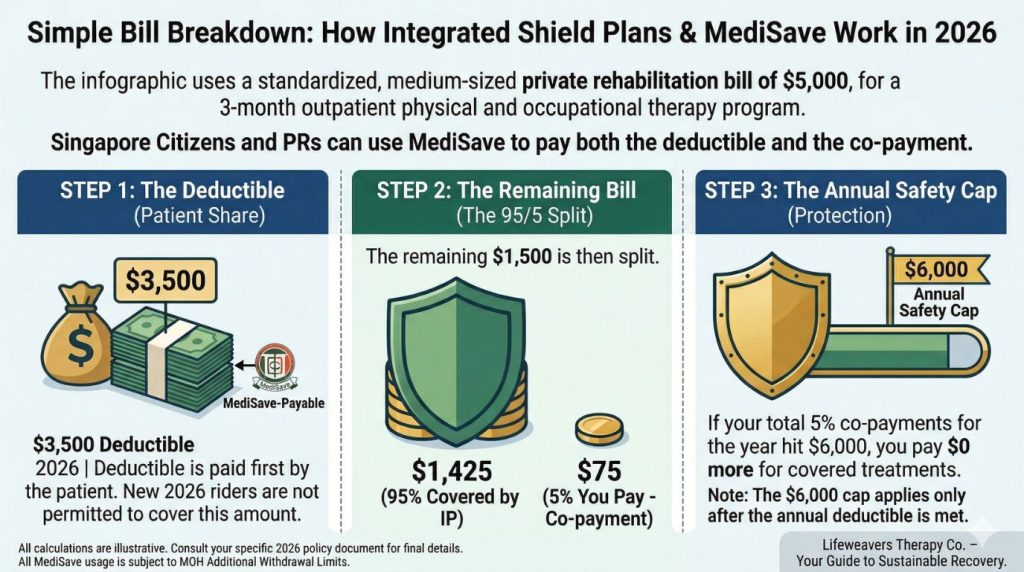
No More Zero-Deductible Riders: Policyholders must now bear the “Deductible” (the first $1,500 to $3,500 of a bill) before insurance kicks in.
The 5% Co-payment: For the remaining bill, you are responsible for a 5% co-payment.
The $6,000 Safety Cap: To protect families from catastrophic costs, your 5% co-payment is capped at $6,000 per year, provided you use Panel Providers and obtain Pre-Authorisation.
Strategic Note: Choosing a rehab provider that coordinates with your insurer’s panel is the only way to guarantee your out-of-pocket costs remain capped.
Home-Based vs. Clinic Rehab: What’s Covered?
In 2026, where you receive therapy is as important as the therapy itself.
Clinic-Based Rehab: Usually treated as standard “outpatient specialist” care and is highly claimable under most IP post-hospitalisation benefits.
Home-Based Rehab: Previously difficult to claim, 2026 Deluxe IP Riders now increasingly recognise Home-Based Rehabilitative Care as a claimable expense, acknowledging that recovery is often most effective in the patient’s natural environment.
Advanced Robotics: High-tech rehab (like robotic gloves or walking aids) is covered if your specialist provides a memo justifying “Medical Necessity.”
What Insurance Doesn’t Cover: Common Pitfalls
Avoid these common “claims traps” to ensure your recovery isn’t interrupted by financial disputes:
The “Maintenance” Plateau: Insurance is designed for “restorative” care. Once a patient reaches a plateau and is only “maintaining” their status, insurers may stop covering sessions.
Self-Referral Without a Specialist: You cannot claim insurance for rehab unless you have a formal referral from a Singapore-registered specialist (e.g., a Neurologist or Orthopaedic Surgeon) following a hospital admission.
Experimental or Wellness Treatments: While TCM is a core part of the Lifeweavers approach, general “wellness” massages are rarely covered unless they are part of a clinical, physician-approved rehab plan.
Closing the Rehab Gap with Lifeweavers
At Lifeweavers, we don’t just provide therapy; we manage your recovery ecosystem. We understand that navigating insurance while recovering from a serious illness is exhausting for families.
Our team assists you by:
Navigating the claims reimbursement process with major Singapore insurers.
Providing the detailed Clinical Progress Reports required for insurance renewals.
Transitioning care from expensive inpatient wards to cost-effective, high-intensity Home or Clinic Recovery.
- You find all the rehab therapists that matters all in the same team, reducing fragmentation of your care and healthcare experience. This is how we make a great difference.
Don’t Let Costs Dictate Your Healthspan
Plan early if you are reading this during good health. Get ample coverage – and in this case, get your Integrated Shield Plans activated. The difference between a partial recovery and a full return to life often comes down to the intensity of early intervention.
Book an Insurance Clarity Consultation: Speak with our care coordinators today to review your 2026 policy limits and ensure your family has the widest range of options for the future.